Murray 2009 Genome Med
| Murray AJ (2009) Metabolic adaptation of skeletal muscle to high altitude hypoxia: how new technologies could resolve the controversies. Genome Med 1:117. https://doi.org/10.1186/gm117 |
Murray AJ (2009) Genome Med
Abstract: In most tissues of the body, cellular ATP production predominantly occurs via mitochondrial oxidative phosphorylation of reduced intermediates, which are in turn derived from substrates such as glucose and fatty acids. In order to maintain ATP homeostasis, and therefore cellular function, the mitochondria require a constant supply of fuels and oxygen. In many disease states, or in healthy individuals at altitude, tissue oxygen levels fall and the cell must meet this hypoxic challenge to maintain energetics and limit oxidative stress. In humans at altitude and patients with respiratory disease, loss of skeletal muscle mitochondrial density is a consistent finding. Recent studies that have used cultured cells and genetic mouse models have elucidated a number of elegant adaptations that allow cells with a diminished mitochondrial population to function effectively in hypoxia. This article reviews these findings alongside studies of hypoxic human skeletal muscle, putting them into the context of whole-body physiology and acclimatization to high-altitude hypoxia. A number of current controversies are highlighted, which may eventually be resolved by a systems physiology approach that considers the time-or tissue-dependent nature of some adaptive responses. Future studies using high-throughput metabolomic, transcriptomic, and proteomic technologies to investigate hypoxic skeletal muscle in humans and animal models could resolve many of these controversies, and a case is therefore made for the integration of resulting data into computational models that account for factors such as duration and extent of hypoxic exposure, subjects' backgrounds, and whether data have been acquired from active or sedentary individuals. An integrated and more quantitative understanding of the body's metabolic response to hypoxia and the conditions under which adaptive processes occur could reveal much about the ways that tissues function in the very many disease states where hypoxia is a critical factor.
• Bioblast editor: Gnaiger E
Labels:
Stress:Hypoxia
Regulation: Substrate
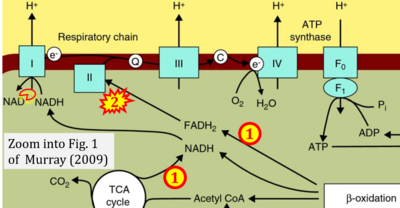
Correction: FADH2 and Complex II
- FADH2 is shown as the substrate feeding electrons into Complex II (CII). This is wrong and requires correction - for details see Gnaiger (2024).
- Gnaiger E (2024) Complex II ambiguities ― FADH2 in the electron transfer system. J Biol Chem 300:105470. https://doi.org/10.1016/j.jbc.2023.105470 - »Bioblast link«
Hydrogen ion ambiguities in the electron transfer system
Communicated by Gnaiger E (2023-10-08) last update 2023-11-10
- Electron (e-) transfer linked to hydrogen ion (hydron; H+) transfer is a fundamental concept in the field of bioenergetics, critical for understanding redox-coupled energy transformations.
- However, the current literature contains inconsistencies regarding H+ formation on the negative side of bioenergetic membranes, such as the matrix side of the mitochondrial inner membrane, when NADH is oxidized during oxidative phosphorylation (OXPHOS). Ambiguities arise when examining the oxidation of NADH by respiratory Complex I or succinate by Complex II.
- Oxidation of NADH or succinate involves a two-electron transfer of 2{H++e-} to FMN or FAD, respectively. Figures indicating a single electron e- transferred from NADH or succinate lack accuracy.
- The oxidized NAD+ is distinguished from NAD indicating nicotinamide adenine dinucleotide independent of oxidation state.
- NADH + H+ → NAD+ +2{H++e-} is the oxidation half-reaction in this H+-linked electron transfer represented as 2{H++e-} (Gnaiger 2023). Putative H+ formation shown as NADH → NAD+ + H+ conflicts with chemiosmotic coupling stoichiometries between H+ translocation across the coupling membrane and electron transfer to oxygen. Ensuring clarity in this complex field is imperative to tackle the apparent ambiguity crisis and prevent confusion, particularly in light of the increasing number of interdisciplinary publications on bioenergetics concerning diagnostic and clinical applications of OXPHOS analysis.